Case report/รายงานผู้ป่วยน่าสนใจ
Emergency Department , Prince of Songkla University, Hadyai, Songkhla; Thailand
Introduction
Pneumopericardium is rare condition and spontaneous pneumopericardium is extremely rare. In reviewing the literature, we found mention of physical exertion1, acute asthma2, cocaine-induced3,episode of weight lifting4 ,passenger on commercial flight5.
We report the unique case of the patient with idiopathic pneumopericardium at rest, which has never been reported before. Our patient recovered without treatment and had no recurrence of pneumopericardium during follow up.
Case report
A 24-year-old, previously healthy woman presented to the emergency department in March 2008 due to Left-sided chest pain radiated to the neck for a week. She denied history of cough, lifting heavy objects or flight at the onset of symptoms.
A week before presentation, she went to Hadyai Hospital and was diagnosed “Myalgia”, after she received diclofenac orally, the clinical condition did not improved.
At the day of presentation, she complaint only left side chest pain while took deep breath, no dyspnea, no cough, no fever.
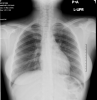
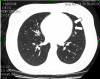
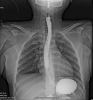
On examination she was look well. Her pulse rate was 92 beats/min, blood pressure was 100/67 mmHg, respiratory rate was 20 breaths/min, and oxygen saturation was 99 % on room air. Chest examination was normal, no subcutaneous emphysema and normal heart sound. A 12-lead electrocardiogram showed normal sinus rhythm. Chest X-ray demonstrated a pneumopericardium (Fig. 1) which was confirmed by computed tomography (Fig 2). The routing laboratory tests were also unremarkable. There was no evidence of other abnormalities. Gastrografin swallow show no leak or any other abnormality (Fig. 3)
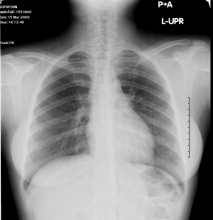
Fig 1: Spontaneous pneumopericardium was show as a radiolucency band at Left heart boarder (arrows)
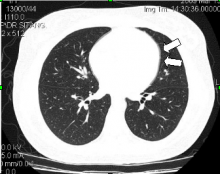
Fig 2: Computed tomography reveals minimal amount of pneumopericardium (arrows).
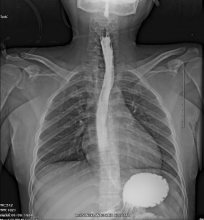
Fig 3: Gastrografin swallow reveals no abnormal extravasation of contrast media.
Without special supportive treatment such as sedation, analgesic or antibiotics and no interventions such as pericardiocentesis were necessary. Repeated chest films in 2 days later, show progressive resolved of the air in the pericardial sac and the patient was discharged. There was no recurrence of pneumopericardium during follow up.
Discussion
Pneumopericardium is rare, defined as a collection of air or gas in the pericardial space and was first described by Bricketeau in 188431.
The amount of air required to produce hemodynamic changes depends on the volume and rate of introduction :
Haemodynamic changes may occur with as little as 60 ml of air if it is introduced rapidly
Up to 500 ml may accumulate into pericardium without marked effect if introduced slowly in the pericardial space7.
Etiology can be devided in to four broad categories. (1)Most common cause is iatrogenic, include following a thoraccentesis, esophagoenterostomy, post-sternal bone marrow aspiration, cardiothoracic surgery or pericardiocenteisis7. In pre term infants during treatment of idiopathic respiratory distress syndrome, the use of positive-pressure ventilation is an important cause8. (2) Trauma, either penetrating chest trauma9-13 or blunt chest trauma14-19. (3) Pericarditis and production of gas caused by gas-forming organisms such as Clostridium perfringens and Klebsiella have been described20,21. It can also occur by direct extension of an inflammatory process such as lung, liver or subphrenic abscess.(4) Fistula formation between the pericardium and air containing structures such as gastrointestinal tract, the pleural cavity and the bronchial tree24-27.
Symptoms of pneumopericardium include chest pain, dyspnea, cyanosis, hypotension, bradycardia or tachycardia and pulsus paradoxus, but are not always present and depend on the extent of pneumopericardium and the underlying disease30. Clinical signs such as distant heart sounds, shifting precordial tympany, and a splashing with metallic tinkling (referred to as the mill wheel murmur, or “bruit de Moulin”) in hydropneumopericardium which was first describe by Bricketeau in 188431. An ECG findings such as low voltage, ST segment changes, and T wave inversion are non-specific and unreliable27,32,33.
Radiographic findings of pneumopericardium and pneumomediastinum can be similar, such as continuous diaphragmatic sign30. Some radiographic signs may help differentiate pneumopericardium from pneumomediastinum, although for pathophysiological reasons, both can coincide. Air outlining the aortic arch, the superior venacava above the azygos vein, or the distal left pulmonary artery are outside the pericardium34. Gas surrounding the heart may be confused with pneumomediastinum27. Therefore a left side down decubitus are helpful to distinguish, since air in pericardial sac will show rapid shift while air in mediastinum will not move in the short interval between films35. The transverse band of air sign (air in the transverse sinus of the pericardium32,35) and the triangle of air sign (a hyperlucency behind the sternum, anterior to the cardiac base and the aortic root32,35) are useful in distinguish pneumopericardium form pneumomediastinum.
It has been suggested that shearing force rupturing the marginal alveolar bases, dissecting the peribronchial and perivascular sheaths with resulting escape of air towards either the pleural space, the hilum or both, are involved in the pathogenesis of pneumothorax and pneumomediastinum. Air spreading peripherally along the pulmonary arteries and veins dissecting through the pericardium along these vessels can result in pneumopericardium2.
The recognition of pneumopericardium and pneumomediastinum are the presence of a history consistent with pericarditis and pain on deep breathing. In the absence of any obvious underlying cause, a history of recent exertion, especially that involving a Valsalva maneuver, should be sought. Mistaking this presentation for pericarditis would lead to an error in therapy, since such cases of spontaneous or idiopathic pneumopericardium are usually associated with small amount of air and have and excellent prognosis with conservative treatment4.
Clinical differential diagnoses include angina pectoris, myocardial infarction, aortic dissection, pericarditis, pneumonitis, pneumothorax, and pulmonary embolism37. A life-treatening tension pneumopericardium can be complication that can be caused by a valve mechanism that allows the air to enter the pericardial sac but not to exit it38. Cardiac temponade then results in decreased cardiac output and circulatory failure27,29. Pneumopericardium can accompanied by subcutaneous emphysema, pneumomediastinum, pneumothorax, and pneumoperitoneum27,28,37.
Treatment of tension and symptomatic pneumopericardium is true emergency condition, immediate needle aspiration and insertion of tube for continuous pericardial drainage is required27,32. Surgical intervention such as emergency thoracotomy and pericardiotomy are needed in some cases27. Oxygen therapy at high concentration can support the absorption of the air36.
A small pneumopericardium without symptoms can be conservative treat by bed rest, observation, sedation, analgesics, antibiotics, because the air will be absorbed spontaneously within a day to week, as in our case1-5,29.
References
1.Gerald W. Westermann and Barbara Suwelack. Spontaneous pneumopericardium due to exertion. South Med J 2003; 96:50-52
2.Toledo TM, Moore WL Jr, Nash DA, et al. Spontaneous pneumopericardium in acute asthma: case report and review of literature. Chest 1972; 62:118-120
3.Carlos A. Albrecht, Abbas Jafri, Lisa Linville and H. Vernon Anderson. Cocaine-induced pneumopericardium. Circulation 2000; 102:2792-2794
4.Baum RS, Welch TG, Bryson AL: Spontaneous pneumopericardium. West J Med 1976;125:154-156
5.Nicol E, Davies G, Jayakumar P, Green NDC. Pneumopericardium and pneumomediastinum in a passenger on a commercial flight. Aviat Space Environ Med 2007; 78:435-439
6.Stacey S et al. A case of spontaneous tension pneumopericardium. Br J Cardiol 2004; 11:14-32
7.Maki DD, Sehgal M, Kricun ME, Gefter WB. Spontaneous tension pneumopericardium complicating staphylococcal pneumonia. J Thorac Imag 1999; 14:215-217
8.Maximo H. Trujillo. Cardiac Tamponade due to pneumopericardium. Cardio 2006; 105:34-36
9.Demetriades D, Charalambides D, Pantanowitz D, Lakhoo M. Pneumopericardium following penetrating chest injuries. Arch Surg 1990; 125:1187-1189
10.Knottenbelt JD, Divaris S. Tension pneumopericardium following stab wounds to the chest: a report of two cases. Injury 1989; 20:46-48
11.Demetriades D, Levy R, Hatzitheofilou C, Chun R. Tension pneumopericardium following penetrating chest injury. J Trauma-Injury Crit Care 1990; 30:238-239
12.Spontnitz AJ, Kaufman JL. Tension pneumopericardium following penetrating chest injury. J Trauma-injury Crit Care 1987; 27:806-808
13.Robinson MD, Markovchick VJ. Traumatic tension pneumopericardium: a case report and literature review. J Emerg Med 1985; 2:409-413
14.Gould JC, Schurr MA. Tension pneumopericardium after blunt chest trauma. Ann Thorac Surg 2001; 72:1730-1738
15.McDougal CB, Mulder GA, Hoffman JR. Tension pneumopericardium following blunt chest trauma. Ann Emerg Med 1985; 14:167-170
16.Hudgens S, McGraw J, Craun M. Two case of tension pneumopericardium following blunt chest injury. J Trauma-Injury Crit Care 1991; 31:1408-1410
17.Capizzi PJ, Martin M, Bannon MP. Tension pneumopericardium following blunt injury. J Trauma-Injury Crit Care 1985; 39:775-780
18.V.V Chitre, M.S.,F.R.C.S.,P.R. Prinsley, F.R.C.S,S.M.H. Hashmi. Pneumopericardium: An unusuaul manifestation of blunt tracheal trauma. J of Laryng & Oto 1997; 111:387-388
19.Thierry C. Roth and Ralph A. Schmid. J Thorac Cardiovas Surg 2002; 124:630-631
20.Ivey,MJ, Gross BH. Back pain and fever in the elderly patient. Chest 1993; 103:1851-1853
21.Tsi WC, Lin LJ, Chen JH, Wu MH. A febrile spontaneous pneumopericardium. Int J Cardiol 1996; 54:69-72
22.Kemal Arda, MD, Olcay Eldem, MD. Spontaneous pneumopericardium and pneumomediastinum. Asian Cardiovasc Thorac Ann 2000; 8:59-61
23.A A Gossage, P W Robertson and S F Stephenson. Spontaneous pneumopericardium. Thorax 1976; 31:460-465
24.Dickson DSP, Girling-Butcher M. Spontaneous pneumopericardium. NZ Med J 1960; 59:250
25.Katzir D,Klinovsky E, Kent V, Shucri A, Gilboa Y. Spontaneous pneumopericardium: case report and review of literature. Cardiology 1989;76:305-308
26.Hsin-Hui Huang, Si-Wa Chan, Yeu-Sheng Tyan. Pneumopericardium caused by perforation of gastrictube after esophageal reconstruction: case report. Chin J Radiol 2006; 31:183-188
27.T M Grandhi, D Rawlings, C G Morran. Gastropericardial fistula: a case report and review of literature. Emerg Med J 2004; 21:644-645
28.Ahmed JM, Salame MY, Oakley GD. Chest pain in a youngirk, Post-grad Med J 1998; 74:115-116
29.Toledo TM, Moore WL Jr, Nash DA, et al. Spontaneous pneumopericardium in acute asthma: case report and review of literature. Chest 1972; 62:118-120
30.L Brander, D Ramsay, D Dreier, M Peter, R Graeni. Continuous left hemidiaphragm sign revisited: a case of spontaneous pneumopericardium and literature review. Heart 2002; 88:e5
31.Bricketeau M. Observation d̒ hydropneumopѐricarde accompagnѐ ď un bruit de fluctuation perceptible a ĺ Oreille. Arch Gen Med 1844; 4:334
32.Capizzi PJ, Martin M, Bannon MP. Tension pneumopericardium following blunt injury. J Trauma 1995; 39:775-780
33.Leitman BS, Greengart A, Wasser HJ. Pneumomediastinum and pneumopericardium after cocaine abuse. AJR AM J Roentgenol 1988; 151;614
34.Bejvan SM, Godwin DJ. Pneumomediastinum: old signs and new signs. Am J Roentgenol 1996; 166:1041-1048
35.Van Gelderen WF. Stab wounds of the heart: Two new signs of pneumopericardium. Br J Radiol 1993; 66:794-796
36.Pomerance JJ, Weller MH, Richardson CJ, Soule JA, Cato A. Pneumopericardium complicating respiratory distress syndrome: Role of conservative treatment. J Pediatr 1974; 84:883-886
37.Luby BJ, Georgiev M, Warren SG, Capito R. Postpartum pneumopericardium. Obstet Gynecol 1983; 62(3 Suppl):46s-50s
Costa IV, Soto B, Diethelm L, Zarco P. Air pericardial temponade. Am J Cardiol 1987;60:1421-1422